The horrors of America’s epidemic of opioid abuse obscure the reason why victims even began taking the very pharmaceuticals which eventually killed them. It was bodily pain – which means any attempt to squelch the opioids plague also must find effective ways to alleviate physical suffering.
To that end, field training by Dr. Joan Broderick, Senior Behavioral Scientist, USC Center for Social & Economic Research, is spreading the word among Los Angeles-area health care professionals about an evidence-based, non-drug approach to managing chronic pain that’s proven to be a success: Pain Coping Skills Training (PCST). Before coming to the University of Southern California, Dr. Broderick and her team had successfully trained close to 40 Advanced Practice nurses in PCST in New York.
Developed over the last 20 years, PCST is a set of strategies and skills that can be taught to those suffering from pain, fatigue, and the emotional upset that comes with chronic pain conditions. Research has demonstrated that when patients are taught these skills, they use less medication and their quality of life improves.
To get this information to those who need it most, Dr. Broderick and her team, with support from the California Health Care Foundation, have taught PCST to nearly 80 health care providers in Los Angeles. The training was open to all team members working with pain patients, including physicians, physicians’ assistants, nurses, social workers, occupational and physical therapists, psychologists, and rehab peer mentors.
The Toll of Pain
Stemming the problem of pain in America would have immense benefits to society, considering that according to the National Institutes of Health more than 1 in 10 Americans suffer chronic pain.
For one, chronic pain is linked to early mortality. At the recent CESR-hosted conference The Future of Inequality, Princeton researchers Anne Case and Sir Angus Deaton discussed the impact of the opioid crisis on particular segments of society. They reported that over the last 20 years, there has been a rising mortality rate for middle-aged, non-Hispanic white men compared with other groups of people. Opioid-related deaths, suicide, and drug/alcohol deaths have made a significant contribution to this. They noted that not only were these people struggling with chronic pain, but intertwined were high rates of stagnant wages or unemployment as well as failed long-term loving relationships.
Of course, pain also elicits an economic price for the nation. The annual cost of pain in America in 2010 was between $560 billion to $635 billion, which exceeded the annual costs of heart disease ($309 billion), cancer ($243 billion), and diabetes ($188 billion).
In response, federal, state and health care system initiatives have been implemented to reduce opioid prescribing. These initiatives will save lives. However, for some patients left without their opioids, they seek alternative “treatment”, including black market pain pills as well as other drugs like heroin. Heath care providers are searching for safer treatments to help their pain patients.
Teaching the Teachers of PCST
Broderick’s training workshop is designed with both didactic presentations of each of the PCST skills followed by practice sessions to give providers a chance to role-play delivery of the skill to a patient. Almost all of the providers (94 percent) rated the training as worthwhile, with 71 percent delivering the grade of “excellent.”
Because assessing the training’s impact on health care providers and their patients has been important to the CHCF, Broderick’s team designed a survey of 29 providers who attended the second of two workshops in 2017. In a 12-week span following a PCST workshop, the survey found that those providers included PCST interventions in more than 900 patient encounters. Of that total, more than 450 patients received Motivational Interviewing and/or Brief Action Planning to begin the shift toward focusing on improved self-management of their condition. In addition, over 325 patients were taught a specific PCST strategy. These interventions were used by providers specifically for reducing opioid use in 100-plus patients. Furthermore, physicians referred more than 125 patients to other members of their team for PCST treatment.
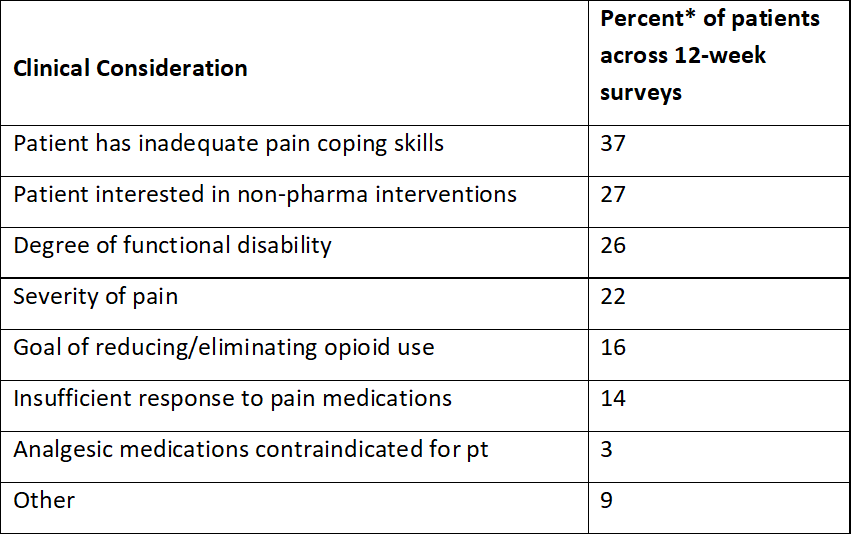
The weekly survey also asked providers to give their reasons for using PCST interventions with their patients. The most frequent reasons reflected recognition of patients’ lack of self-management skills, pain’s negative impact on daily functioning, and level of residual pain despite conventional treatment. The providers said more than a quarter of their patients requested their treatment plans include non-pharmaceutical approaches. Providers also said they used PCST strategies for pain-related symptoms such as sleep disturbance, interference with daily functioning, benzodiazepine dependence, and weight reduction, as well as comorbid conditions such as diabetes. This all suggests a robust uptake of PCST for treating patients with chronic pain.
Obstacles to Adoption
Alongside these successes, the PCST-trained providers also described systemic challenges to using non-pharmaceutical approaches with their patients, chief among them limited time. Writing a prescription for opioids and other pain medications takes just a moment, while introducing and training patients in new skills to manage their pain takes more time – at least in the short term – and most providers struggled with finding those opportunities in their tight clinic schedules. This same issue also hindered providers’ ability to follow up on patients’ use of these new strategies at home. For many patients, a shift away from focusing on medication as the primary treatment requires time and support to make this transition successfully. In some cases, this was dealt with by referring patients to providers on their team (e.g., social workers, occupational therapists) who typically can spend more time with patients or by creating group training opportunities for patients. They also requested further training opportunities to deepen their expertise in non-pharmaceutical approaches.
You must be logged in to post a comment.